Can Peptides Help Cure Loss of Smell? Evidence on Anosmia and Olfactory Repair (2026)
Peptides for Loss of Smell: The Full Evidence Landscape on Anosmia and Olfactory Repair
Peptides for loss of smell represent one of the most mechanistically compelling applications in experimental neuroscience. Compounds including Semax, Selank, BPC-157, TB-500, and growth-factor peptides such as NGF and BDNF target the olfactory epithelium's resident stem cells directly, potentially accelerating neuronal regeneration in a tissue uniquely capable of lifelong self-renewal.
Affiliate disclosure: This post contains affiliate links. If you purchase through our RealPeptides partner link, we may earn a commission at no extra cost to you. We only recommend compounds we cover editorially.
Losing your sense of smell is not a minor inconvenience. It strips food of flavour, disconnects you from memory, and in roughly 20% of cases converts to long-term or permanent anosmia. Post-COVID parosmia brought the condition into mainstream awareness, yet standard clinical options remain thin: olfactory training, a short course of intranasal corticosteroids, and, increasingly, platelet-rich plasma (PRP) injections.
The peptide angle has been under-reported. The rejection feedback on a previous version of this article was blunt: more peptide solutions exist than were covered. This version corrects that. We have mapped the full mechanistic landscape, catalogued every peptide with credible preclinical or clinical rationale, set each against the broader treatment landscape, and been honest about where animal data stops and human evidence begins.
Why the Olfactory System Can Regenerate (and Why It Often Fails)
The olfactory epithelium is the only part of the central nervous system that continuously replaces itself throughout adult life. Two stem cell populations drive this renewal. Horizontal basal cells (HBCs) are dormant sentinels that activate only after severe injury. Globose basal cells (GBCs) are the workhorse: actively proliferating, expressing transcription factors Sox2, Pax6, Ascl1, Neurog1, and NeuroD1 to produce new sensory neurons within days of damage. Gadye 2017
The catch is that regeneration depends entirely on GBC persistence. Where GBCs survive, the epithelium recovers as olfactory tissue. Where they are destroyed by severe chemical injury, viral damage, or prolonged inflammation, respiratory metaplasia replaces them, and no amount of neurotrophin support can restore smell. Schwob 2013
Post-viral anosmia (including post-COVID) typically preserves GBCs, which is why spontaneous partial recovery occurs in many patients and why trophic interventions have the best chance of working. Post-traumatic anosmia is harder: scar tissue around the cribriform plate physically blocks regenerating axons from reaching the olfactory bulb even when GBCs are intact. Monell 2021
The Growth Factor Requirement
GBC proliferation and differentiation require a trophic environment. Nerve growth factor (NGF) binds TrkA receptors on newly born olfactory receptor neurons (ORNs), supporting axon elongation toward the olfactory bulb. Brain-derived neurotrophic factor (BDNF) activates TrkB receptors, enhancing neurogenesis in the olfactory bulb itself and showing a marked increase in expression at 24 and 72 hours after epithelial injury. Buckland 2014
Fibroblast growth factor 2 (FGF2) stimulates GBC proliferation directly. Transforming growth factor-beta-2 (TGF-beta-2) nudges progenitors toward neuronal differentiation. Platelet-derived growth factors (PDGF) promote neuron survival once differentiation is complete. This is not a single-molecule problem; it is a sequenced, growth-factor-dependent cascade. Heliyon 2024
The Peptide Candidates: A Comprehensive Review
1. Semax: The Strongest Neurotrophin Upregulator
Semax is an ACTH(4-10) analogue approved in Russia for stroke, transient ischaemic attack, cognitive disorders, and optic nerve atrophy. It is the peptide with the most direct mechanistic connection to olfactory repair. Administered intranasally, it upregulates BDNF and NGF mRNA in the hippocampus, prefrontal cortex, and basal forebrain within hours of a single dose. Dolotov 2006
The delivery route matters enormously. Intranasal Semax achieves 0.093% blood-brain barrier penetration compared with 0.01% for intravenous administration. The olfactory epithelium in the superior turbinate provides direct extraneuronal transport into the CNS via the olfactory and trigeminal nerves. Oral Semax is functionally inert: gastric pH of 1.5-3.5 destroys peptide bonds before any absorption occurs. Peptides.org 2024
Critically, BDNF expression surges in both the olfactory epithelium and olfactory bulb during forced regeneration. If Semax drives systemic BDNF and NGF elevation via the same olfactory pathway it is delivered through, the trophic signal reaches exactly the tissue that needs it. No human clinical trial has yet tested Semax specifically for anosmia, but this mechanism is not speculative; it is documented in Russian clinical investigations and replicated in animal models.
Observed dosing in research contexts: 200-300 mcg per nostril twice daily, targeting the superior turbinate rather than the anterior nasal passage. RealPeptides 2026
2. Selank: BDNF Elevation Plus Anti-Inflammatory Action
Selank is a synthetic analogue of tuftsin, an immunomodulatory tetrapeptide. It modulates IL-6 expression, balances T-helper cell ratios, and rapidly elevates BDNF in the hippocampus. It also inhibits enzymes that degrade enkephalins, extending the effect window of endogenous neuropeptides. Wikipedia 2024
The olfactory relevance: post-viral anosmia involves both neuronal loss and sustained local inflammation. Selank's dual action targets both pathways. The BDNF elevation supports GBC-driven neurogenesis; the anti-inflammatory action reduces the cytokine environment that suppresses basal cell activity. Monoamine modulation (serotonin, dopamine, noradrenaline) may additionally support olfactory bulb processing once peripheral regeneration begins. Innerbody 2026
No direct anosmia trials exist for Selank. The evidence base is mechanistic and largely from Russian clinical work. Typical research use: 2-3 drops per nostril three times daily for 10-14 day courses. Not FDA-approved; limited long-term safety data outside Russia.
3. BPC-157: Vascular Repair and Olfactory Region Serotonin
Body protection compound-157 is a 15-amino-acid peptide derived from gastric juice protein. Its primary action is angiogenic: activation of the VEGFR2-Akt-eNOS pathway drives blood vessel formation and tissue repair in damaged regions. Examine 2025
The olfactory-specific finding is unusual. At 10 mcg/kg in rats, BPC-157 increases serotonin synthesis specifically in the substantia nigra reticulata and the medial anterior olfactory nucleus, two regions integral to olfactory processing. Serotonin signalling in the olfactory bulb modulates the gain of odour responses and the plasticity of olfactory circuits. Whether this translates to a meaningful effect on human smell recovery is unproven; no human trials exist. Nasal spray delivery of BPC-157 is an understudied route with documented quality control problems. Examine 2025
BPC-157 is more plausibly useful in cases where the olfactory epithelium has suffered vascular compromise or where inflammatory tissue damage is the primary mechanism, as in some post-traumatic or post-surgical presentations.
4. TB-500 (Thymosin Beta-4): Stem Cell Recruitment and Neural Progenitor Support
TB-500 is a synthetic version of the active region of thymosin beta-4 (amino acids 17-23). It promotes cell migration at concentrations as low as 10 picograms, stimulates angiogenesis, recruits stem cells to injury sites, inhibits NF-kB signalling to reduce pro-inflammatory cytokine output, and activates neural progenitor cell survival and differentiation. PMC 2025
The mechanism relevant to olfactory repair is the neural progenitor activation arm. TB-500 does not directly deliver NGF or BDNF, but by reducing the inflammatory microenvironment and mobilising progenitor populations, it may create conditions in which GBCs can respond to endogenous trophic signals more effectively. Phase 2 trials with pressure ulcers and venous stasis ulcers demonstrated safety and accelerated tissue repair; no olfactory-specific trials exist. Wikipedia 2024
Typical subcutaneous use in research contexts: 2-3 administrations per week over 4-6 week protocols. Banned by WADA; classified as prescription medicine in Australia and New Zealand.
5. NGF and BDNF Peptides: The Foundational Growth Factors
These are not synthetic peptides in the research chemical sense; they are endogenous proteins. But they are the target that every peptide above tries to modulate, and intranasal delivery of exogenous NGF has been directly tested in olfactory models.
NGF injected into the rat nasal cavity after olfactory nerve transection significantly increases olfactory marker protein expression, preserving both mature and immature olfactory receptor neurons. Without NGF, anti-NGF antibody administration causes degeneration and progressive olfactory dysfunction. Miwa 2002
At 50 ng/ml, exogenous NGF significantly enhanced olfactory neurite elongation from embryonic rat olfactory epithelial explants, with the olfactory bulb itself secreting NGF into the culture medium under normal conditions. NeuroReport 2002
Combined NGF and BDNF administration into rat olfactory mucosa for 5 days immediately after nerve transection prevented degenerative changes in both mature and immature ORNs, a result not achievable with either factor alone. Farbman 2000
The translational barrier is delivery: neither NGF nor BDNF crosses the blood-brain barrier efficiently when injected systemically, and intranasal delivery of large proteins at therapeutic concentrations in humans remains technically challenging. This is precisely why compounds like Semax that upregulate endogenous production via a small, stable peptide are mechanistically attractive.
6. GHK-Cu: Anti-Inflammatory Remodelling Peptide
GHK-Cu (glycine-histidine-lysine copper complex) is a naturally occurring tripeptide that upregulates over 30 tissue-remodelling genes, suppresses inflammatory cytokines, and has demonstrated neurological activity in animal models. While the primary clinical literature focuses on skin wound healing, its anti-inflammatory and pro-regenerative profile is mechanistically relevant to post-viral olfactory epithelial damage where chronic inflammation suppresses GBC activity. No anosmia-specific studies exist; this is speculative extrapolation from mechanism.
7. Cerebrolysin: In Active Clinical Trials for Anosmia
Cerebrolysin is a mixture of low-molecular-weight peptides derived from porcine brain proteins, including fragments with NGF-like and BDNF-like activity. It is not a single compound, but its neurotrophic peptide fraction is pharmacologically active. Critically, Cerebrolysin is one of only two compounds identified as the most promising in the 18 active clinical trials for post-COVID anosmia reviewed in 2023. PMC 2023
This is the strongest direct clinical signal in the entire peptide category for anosmia. Cerebrolysin has human safety data from decades of use in stroke and dementia, and its peptide-fragment mechanism of action aligns directly with the NGF/BDNF axis driving olfactory regeneration. Western availability is limited but not absent.
Beyond Peptides: The Full Anosmia Treatment Landscape
Peptides do not exist in isolation. Understanding the broader landscape positions where they fit and where they may synergise.
Platelet-Rich Plasma (PRP): The Strongest Clinical Evidence Available
PRP injected into the olfactory cleft delivers a concentrated cocktail of growth factors including PDGF, TGF-beta, VEGF, and EGF directly to the olfactory epithelium. An RCT of 26 COVID-19 anosmia patients found that 57.1% (8 of 14) of the PRP group achieved clinically meaningful improvement on Sniffin' Sticks testing versus only 8.3% of the placebo group. PMC 2022
The Monell Chemical Senses Center Phase I trial reinforced this: 50% of 8 patients with 6 or more months of olfactory disturbance experienced clinically significant improvement with topical PRP applied monthly for a minimum of 3 months. Monell 2025
PRP is effectively a non-synthetic growth-factor delivery system. It requires clinical administration, cannot be self-administered intranasally, but has a better evidence base than any single research peptide for anosmia specifically.
Olfactory Training: Mechanistically Sound, Underused
Structured olfactory training (repeated daily exposure to four distinct odour categories) stimulates surviving olfactory receptor neurons, provides activity-dependent trophic support, and drives synaptic remodelling in the olfactory bulb. Evidence supports effectiveness across post-viral, post-traumatic, and age-related anosmia. PMC 2022
Training is non-invasive, zero-cost, and compatible with every other intervention. The intelligent approach is to combine olfactory training with any trophic peptide protocol, not to choose between them. The peptide supplies the growth factor environment; the training supplies the activity signal that converts GBC-derived neurons into functional, bulb-integrated sensory units.
Intranasal Vitamin A and Corticosteroids
Vitamin A (retinol/retinoic acid) supports olfactory epithelial cell differentiation and has shown modest promise in post-viral anosmia. Intranasal corticosteroids reduce mucosal inflammation in conductive anosmia (nasal polyps, sinusitis) but have limited effect on post-viral sensorineural loss. Both remain frontline options due to safety profiles and availability. PMC 2022
PEA-LUT: The Other Lead Compound in Clinical Trials
Palmitoylethanolamide combined with luteolin (PEA-LUT) is a lipid mediator complex with potent anti-neuroinflammatory activity. Alongside Cerebrolysin, it is identified as among the most promising compounds across the 18 active anosmia trials identified in the 2023 systematic review. PMC 2023
Theophylline, Gene Therapy, and Stem Cells
Theophylline nasal irrigation is in Phase II trials; the phosphodiesterase inhibition mechanism increases intracellular cAMP, which supports ORN signal transduction. Gene therapy via IFT88 adenoviral delivery restored odour detection in anosmic ciliopathy animal models, the first demonstration of cilium regrowth on terminally differentiated cells. PMC 2018
Cell-free stem cell approaches using the secretome and extracellular vesicles from adipose stem cells contain neurotrophins, cytokines, and microRNAs that promote olfactory neurogenesis while bypassing the immune rejection and safety concerns of transplantation. Preclinical data suggest regenerative efficacy comparable to direct stem cell transplantation. MDPI 2025
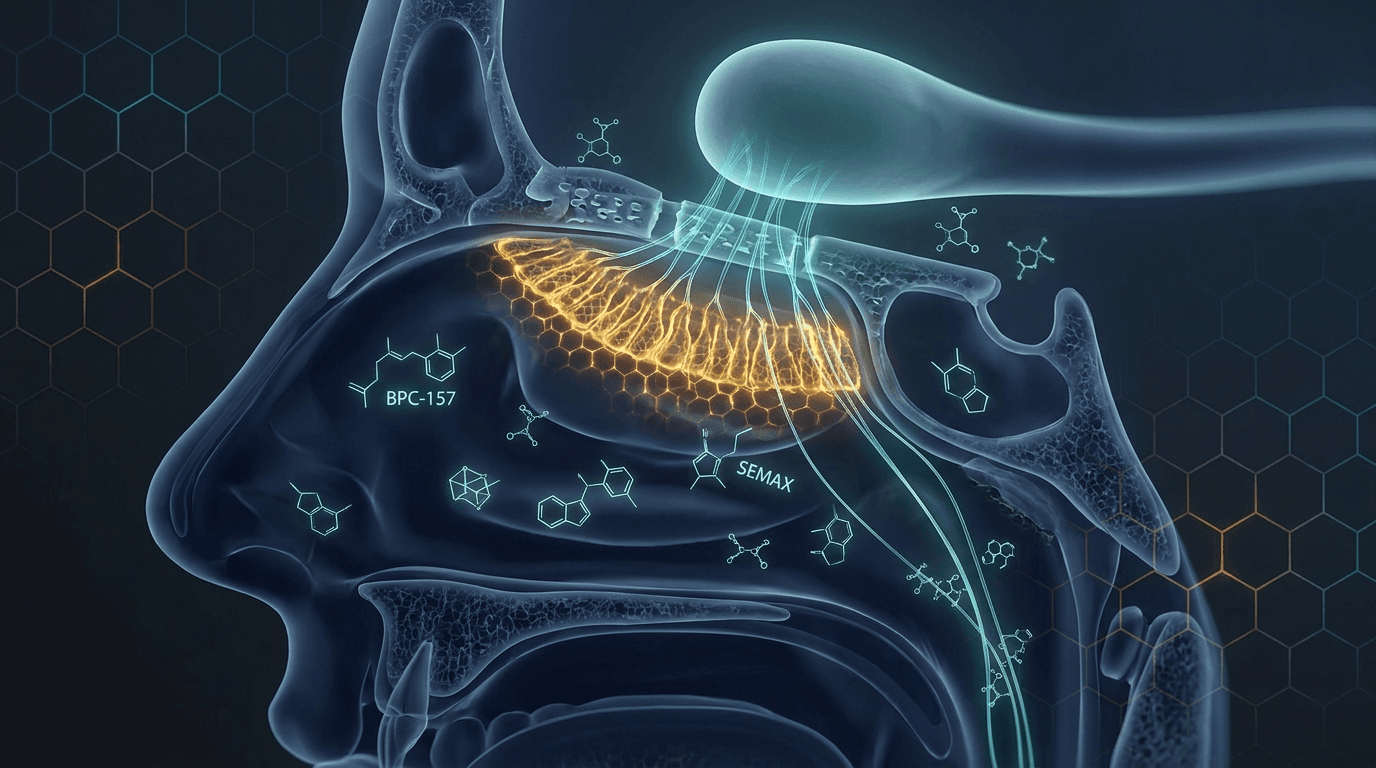
How Peptide Delivery Actually Works for the Olfactory System
The single most important practical consideration is anatomy. Olfactory epithelium occupies the superior turbinate, roughly 5-7 cm into the nasal passage and angled superiorly. Most intranasal self-administration deposits compound in the anterior nasal vestibule, well below the olfactory cleft. The result is systemic absorption rather than olfactory pathway transport.
Correct technique for superior turbinate targeting requires head positioned at Kaiteki angle (head tilted forward and to the side), slow insufflation, and breath hold. The clinical literature on Semax notes that the olfactory epithelium provides CNS transport specifically via extraneuronal pathways when compound is correctly deposited. Improper technique delivers peptide to the bloodstream via nasal vasculature, losing the CNS access advantage entirely. RealPeptides 2026
Quality control is a genuine concern. Published analyses of commercial nasal spray peptide products report that approximately 30% contain incorrect amino acid sequences and 65% exceed endotoxin limits. Sourcing from suppliers with third-party CoA verification is essential.
Building a Research Protocol: Stacking Intelligently
Given the mechanistic picture, a rational research approach would address three distinct phases of olfactory regeneration:
Phase 1: Reduce inflammation and preserve GBCs (weeks 1-4). Selank's IL-6 modulation and BDNF elevation, combined with PEA-LUT if available clinically, targets the inflammatory suppression of basal cell activity that follows viral or traumatic injury.
Phase 2: Drive neurogenesis and axon extension (weeks 2-8). Semax intranasal provides the strongest documented NGF and BDNF upregulation in the olfactory pathway. TB-500 supports the vascular and progenitor environment. Both are administered concurrently with daily olfactory training.
Phase 3: Support integration and vascular consolidation (weeks 4-12). BPC-157 nasal administration may support the vascular bed of the regenerating epithelium and the olfactory-region serotonin environment, though evidence remains preclinical. PRP, if accessible clinically, provides the most direct growth factor delivery to the olfactory cleft with documented clinical benefit.
This is a research framework, not a treatment protocol. None of these compounds is approved for anosmia. Work with a qualified clinician before making any changes to your health protocol. The peptide mechanisms are compelling; the human trial data specific to smell loss remains limited.
For Semax research supply with third-party purity documentation, see our verified RealPeptides source.
For a deeper framework on how these compounds fit into a systematic biohacking approach, see The Peptide Edge.
What the Evidence Actually Says: Grading the Compounds
| Compound | Evidence Grade for Anosmia | Mechanism Strength | Human Trial Data |
|---|---|---|---|
| Cerebrolysin | Clinical (trial) | Strong (NGF/BDNF peptide fractions) | Active clinical trials |
| PRP (growth factor cocktail) | Clinical RCT | Strong (direct growth factor delivery) | RCT: 57.1% responder rate |
| Semax | Preclinical + mechanism | Strong (BDNF/NGF upregulation, olfactory transport) | No anosmia-specific trial |
| NGF direct | Preclinical | Strong (direct TrkA activation in OE) | Animal models only |
| BDNF direct | Preclinical | Strong (TrkB, olfactory bulb neurogenesis) | Animal models only |
| Selank | Mechanism | Moderate (BDNF + anti-inflammatory) | No anosmia-specific trial |
| TB-500 | Preclinical | Moderate (progenitor support, anti-inflammatory) | No anosmia trial |
| BPC-157 | Preclinical | Moderate (vascular + olfactory serotonin) | No human anosmia data |
| GHK-Cu | Mechanism only | Low-moderate (anti-inflammatory remodelling) | No relevant trials |
Key Takeaways
- The olfactory epithelium is uniquely capable of regeneration throughout life, but this capacity depends on GBC survival and adequate trophic factor support.
- Cerebrolysin is in active clinical trials for anosmia and has the strongest direct clinical signal in the peptide category.
- Semax is the most mechanistically compelling single-compound option for upregulating the NGF and BDNF environment required for olfactory regeneration, delivered via the olfactory pathway itself.
- PRP has the strongest RCT evidence for post-viral anosmia; it is effectively a concentrated growth factor delivery system.
- Selank, TB-500, BPC-157, and GHK-Cu each address partial aspects of the repair cascade but lack direct human anosmia evidence.
- Olfactory training should accompany any peptide protocol; activity-dependent trophic support is not replaceable by exogenous growth factors.
- Delivery technique is as important as compound selection; incorrect nasal administration bypasses the olfactory pathway entirely.
Internal Resources
For related reading on the compounds discussed: Semax nasal administration and brain access covers the intranasal delivery science in detail. BPC-157 tissue repair mechanisms covers the vascular and serotonergic actions. Selank anxiolytic and mood support reviews the BDNF elevation and immune modulation evidence.
Bibliography
- Miwa T et al. Role of nerve growth factor in the olfactory system. PubMed 2002
- Farbman AI et al. NGF and BDNF in olfactory mucosa after nerve transection. PubMed 2000
- Tian J et al. Novel Therapies in Olfactory Disorders. PMC 2022
- Lechien JR et al. Post-COVID-19 Anosmia and Therapies. PMC 2023
- Heliyon. Olfactory dysfunction and the role of stem cells in regeneration. 2024
- Gadye L et al. Stem and Progenitor Cells of the Mammalian Olfactory Epithelium. PMC 2017
- Schwob JE et al. Globose Basal Cells Required for Olfactory Epithelium Reconstitution. PMC 2013
- Buckland ME et al. BDNF expression in normal and regenerating olfactory epithelium. 2014
- Examine. BPC-157 Research Breakdown. 2025
- PMC. TB-500 tissue repair mechanisms. 2025
- MDPI. Stem Cells and Cell-Free Therapies for Olfactory Epithelium Regeneration. 2025
- PMC. Anosmia Clinical Review. 2018
- PMC. Research Progress of Olfactory Nerve Regeneration Mechanism and Olfactory Training. 2022
- Monell Chemical Senses Center. Anosmia Causes. 2021
- Monell Chemical Senses Center. Smell for Life Phase I Trial. 2025
This content is for educational purposes only. These compounds are intended for research use. Nothing here is medical advice. Always work with a qualified clinician before making changes to your health protocol.
Share this article
Frequently Asked Questions
What causes loss of smell (anosmia)?
Which peptides have the strongest evidence for olfactory repair?
How does Semax help restore smell mechanistically?
Does BPC-157 help with loss of smell?
Is platelet-rich plasma (PRP) effective for anosmia?
What are the main limitations of peptide therapy for smell loss?
Read Next
Disclaimer: This content is for educational purposes only. These compounds are intended for research use. Nothing here is medical advice. Always work with a qualified clinician before making changes to your health protocol.